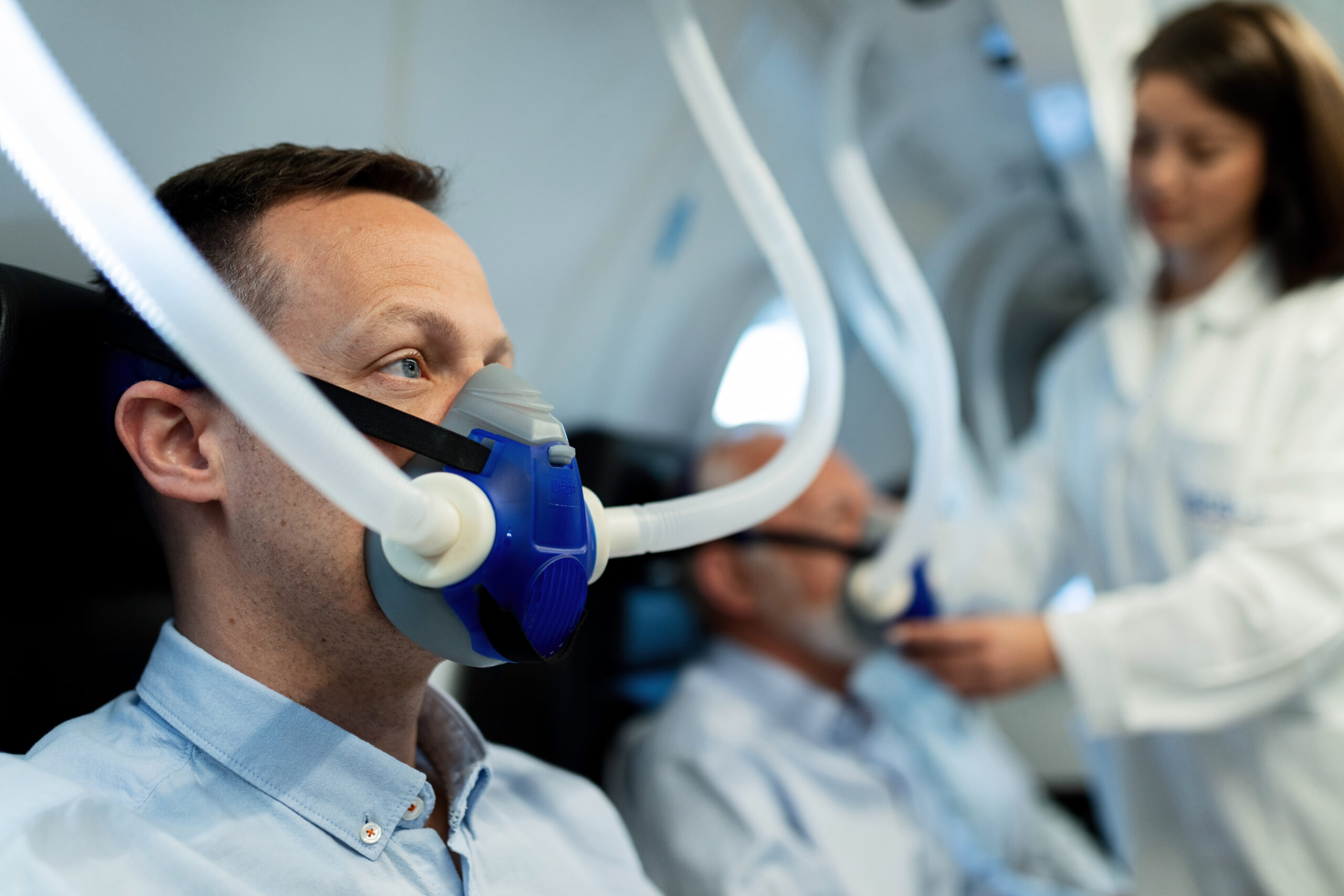
In the realm of sleep disorders, obstructive sleep apnea (OSA) reigns as a prevalent and potentiadlly hazardous condition. With its hallmark characteristic of recurrent upper airway obstruction during sleep, OSA poses challenges not only to restful slumber but also to overall health and well-being. This comprehensive guide aims to illuminate the diverse facets of obstructive sleep apnea, including its various types, symptoms, diagnostic approaches, and an array of treatment modalities.
If you’re struggling with symptoms like loud snoring, daytime sleepiness, or morning headaches, it’s time to take action. Book an appointment with our sleep specialist to start your journey towards a better night’s sleep.
Understanding Obstructive Sleep Apnea:
Obstructive sleep apnea, often abbreviated as OSA, represents the most common form of sleep-disordered breathing. It unfolds as a repetitive sequence of events during sleep, wherein the upper airway becomes partially or completely obstructed, impeding the flow of air into the lungs. This obstruction leads to intermittent episodes of breathing cessation, disrupting the normal sleep pattern and diminishing the quality of rest.
Don’t let obstructive sleep apnea disrupt your life any longer. Call now to schedule your consultation and take the first step towards effective treatment and improved sleep quality.
Within the spectrum of obstructive sleep apnea, distinct categories emerge based on the severity and frequency of apneic episodes. These classifications serve as crucial indicators for treatment strategies and prognostic implications:
- Mild Obstructive Sleep Apnea: Mild OSA, or mild sleep apnea, denotes a condition characterized by infrequent and relatively brief periods of airflow obstruction during sleep. While the manifestations of mild OSA may be less pronounced compared to severe cases, the associated symptoms, such as daytime fatigue and impaired cognitive function, are nonetheless impactful. For some individuals with mild or moderate obstructive sleep apnea, oral devices designed to keep the throat open by bringing the lower jaw forward or holding the tongue in a different position may offer relief. Additionally, a newer device that uses electrical stimulation on the tongue can improve snoring and breathing during sleep in people with very mild sleep apnea and snoring.
- Moderate Obstructive Sleep Apnea: Moderate OSA encompasses a middle ground wherein the frequency and duration of apneic events during sleep are more pronounced than in mild cases. Individuals with moderate OSA often experience heightened daytime sleepiness and may be at an increased risk of developing complications associated with sleep-disordered breathing.
- Severe Obstructive Sleep Apnea: Severe OSA, or severe sleep apnea, represents the apex of the spectrum, characterized by frequent and prolonged episodes of upper airway obstruction during sleep. The repercussions of severe OSA extend beyond mere sleep disturbances, predisposing affected individuals to a myriad of cardiovascular and metabolic comorbidities. For those unable to tolerate CPAP treatment, alternatives such as oral devices and electrical stimulation devices are mentioned, providing potential relief and management options.Ready to tackle obstructive sleep apnea head-on? Contact us today to schedule an appointment and explore personalized treatment options tailored to your needs and preferences.
Symptoms and Clinical Manifestations of Severe Obstructive Sleep Apnea:
The manifestations of obstructive sleep apnea span a broad spectrum, encompassing both nocturnal disturbances and daytime impairments. Key symptoms and clinical manifestations include:
- Loud Snoring: A hallmark feature of OSA, loud and persistent snoring often accompanies episodes of upper airway obstruction during sleep.
- Excessive Daytime Sleepiness: Daytime fatigue and excessive drowsiness represent cardinal symptoms of OSA, stemming from disrupted sleep architecture and recurrent arousals during the night. Untreated obstructive sleep apnea significantly increases the risk of falling asleep during critical activities like driving or operating machinery, which can lead to serious accidents and underscores the danger of falling asleep in such situations.
- Gasping or Choking Episodes: Individuals with OSA may experience episodes of gasping or choking during sleep as the body attempts to overcome the obstruction and restore normal breathing.
- Morning Headaches: Morning headaches are a common complaint among individuals with OSA, attributed to nocturnal hypoxemia and alterations in cerebral blood flow.
- Impaired Cognitive Function: Cognitive deficits, including impaired memory, difficulty concentrating, and reduced attention span, are prevalent among individuals with untreated OSA.
- Mood Disturbances: OSA has been linked to mood disturbances such as irritability, depression, and anxiety, which can further exacerbate daytime impairments.Take charge of your sleep health and well-being. Book your appointment now to discuss your symptoms and explore the best treatment options for managing obstructive sleep apnea effectively.
Diagnosing Obstructive Sleep Apnea:
To diagnose sleep apnea, the process involves participating in a sleep study, undergoing a physical exam, and providing medical history and information about symptoms and bedtime routine. Accurate diagnosis of obstructive sleep apnea necessitates a multifaceted approach encompassing clinical evaluation, objective testing, and assessment of symptomatology. Key components of the diagnostic workup include:
- Comprehensive History and Physical Examination: A thorough clinical history, including evaluation of symptoms such as snoring, witnessed apneas, and daytime sleepiness, lays the foundation for the diagnostic process. Physical examination may reveal anatomical abnormalities predisposing to airway collapse, such as enlarged tonsils, retrognathia, or nasal obstruction.
- Sleep Study (Polysomnography): Polysomnography, often regarded as the gold standard for diagnosing OSA, involves overnight monitoring of physiological parameters during sleep. This comprehensive evaluation encompasses the assessment of respiratory effort, airflow, oxygen saturation, sleep architecture, and arousal, providing valuable insights into the severity and nature of sleep-disordered breathing.
- Home Sleep Apnea Testing (HSAT): Home sleep apnea testing offers a convenient alternative to in-laboratory polysomnography for selected individuals with a high pretest probability of moderate to severe OSA. HSAT typically involves the use of portable monitoring devices to record key respiratory parameters, including airflow, respiratory effort, and oxygen saturation, within the comfort of the patient’s home environment.Say goodbye to restless nights and hello to rejuvenating sleep. Book your appointment today to uncover personalized solutions for managing obstructive sleep apnea and reclaiming quality rest.
Treatment Modalities for Obstructive Sleep Apnea:
Treating obstructive sleep apnea involves a comprehensive approach that includes a variety of treatment options tailored to meet individual patient needs and preferences. From lifestyle modifications to medical interventions and surgical procedures, the therapeutic armamentarium for OSA is expansive and multifaceted:
- Continuous Positive Airway Pressure (CPAP) Therapy: CPAP therapy stands as the cornerstone of treatment for obstructive sleep apnea, offering a non-invasive means of maintaining airway patency during sleep. This modality involves the application of continuous positive airway pressure via a nasal or facial mask, effectively splinting the upper airway and preventing collapse.
- Bi-level Positive Airway Pressure (BiPAP) Therapy: BiPAP therapy, also known as bilevel positive airway pressure, provides distinct pressure settings for inhalation and exhalation, accommodating the respiratory needs of individuals with varying degrees of airway obstruction. This mode of therapy may be particularly beneficial for patients with underlying respiratory muscle weakness or intolerance to CPAP.
- Oral Appliance Therapy: Oral appliances, including mandibular advancement devices and tongue-retaining devices, offer a conservative yet effective means of alleviating upper airway obstruction in select patients with mild to moderate OSA. These custom-fitted devices work by repositioning the mandible or tongue to enhance airway patency during sleep, thereby reducing the frequency and severity of apneic events.
- Surgical Interventions: Surgical interventions play a pivotal role in the management of OSA, especially in cases refractory to conservative measures or those characterized by anatomical abnormalities predisposing to airway collapse. Surgical options may encompass procedures targeting the nasal passages (e.g., septoplasty, turbinate reduction), soft palate (e.g., uvulopalatopharyngoplasty), or upper airway (e.g., genioglossus advancement, hyoid suspension).
- Lifestyle Modifications: Lifestyle modifications, including weight loss, avoidance of alcohol and sedative medications, and positional therapy, constitute integral components of OSA management. Weight loss, in particular, has been shown to significantly improve OSA severity and may lead to partial or complete resolution of symptoms in obese individuals.Embark on your journey towards improved sleep and overall well-being. Schedule your appointment to explore innovative treatments and lifestyle adjustments for combating obstructive sleep apnea. Book online now.
Frequently Asked Questions (FAQs) About Types of Obstructive Sleep Apnea
- What is Obstructive Sleep Apnea?
- Obstructive sleep apnea (OSA) is a common sleep disorder characterized by recurrent episodes of upper airway obstruction during sleep, leading to breathing pauses and disruptions in sleep patterns.
- What are the Different Types of Sleep Apnea?
- Sleep apnea encompasses various types, including obstructive sleep apnea (OSA), central sleep apnea (CSA), and mixed sleep apnea. OSA is the most prevalent form and involves physical obstruction of the airway during sleep.
- How is Obstructive Sleep Apnea Diagnosed?
- Obstructive sleep apnea is diagnosed through a combination of clinical evaluation and diagnostic tests such as polysomnography (sleep study) or home sleep apnea testing. Symptoms, medical history, and physical examination are key components of the diagnostic process.
- What Are the Symptoms of Obstructive Sleep Apnea?
- Symptoms of obstructive sleep apnea include loud snoring, daytime sleepiness, gasping or choking during sleep, morning headaches, irritability, and difficulty concentrating.
- What Causes Obstructive Sleep Apnea to Occur?
- Obstructive sleep apnea occurs when the throat muscles relax excessively during sleep, leading to partial or complete blockage of the airway. Factors such as obesity, anatomical abnormalities, and aging can contribute to airway collapse.
- How is Obstructive Sleep Apnea Treated?
- Treatment options for obstructive sleep apnea include lifestyle modifications, continuous positive airway pressure (CPAP) therapy, oral appliances, surgical interventions, and positional therapy.
- What is Continuous Positive Airway Pressure (CPAP)?
- CPAP therapy involves the use of a machine that delivers a continuous flow of air through a mask worn over the nose or mouth during sleep. This air pressure helps to keep the airway open and prevents episodes of apnea.
- What Are the Risk Factors for Obstructive Sleep Apnea?
- Risk factors for obstructive sleep apnea include obesity, older age, male gender, family history, anatomical abnormalities of the upper airway, and certain medical conditions such as hypertension and diabetes.
- Can Obstructive Sleep Apnea be Prevented?
- While certain risk factors for obstructive sleep apnea cannot be changed, adopting a healthy lifestyle, maintaining a healthy weight, avoiding alcohol and sedatives before bedtime, and sleeping on your side may help reduce the risk of OSA.
- What Are the Consequences of Untreated Obstructive Sleep Apnea?
- Untreated obstructive sleep apnea can lead to serious health consequences, including high blood pressure, heart disease, stroke, diabetes, and daytime fatigue that can impair daily functioning and increase the risk of accidents.Ready to transform your sleep and revitalize your life? Contact us today to schedule your consultation and discover how effective management of obstructive sleep apnea can lead to a brighter, more energized tomorrow.
Conclusion:
Obstructive sleep apnea stands as a pervasive and multifaceted sleep disorder with far-reaching implications for health and quality of life. By delineating the diverse types of OSA, elucidating the spectrum of symptoms and clinical manifestations, and exploring the myriad diagnostic and therapeutic modalities available, this comprehensive guide aims to empower individuals and healthcare providers alike in the journey toward effective management and mitigation of this pervasive sleep disorder. Through a holistic approach encompassing lifestyle modifications, medical interventions, and surgical treatments, individuals with obstructive sleep apnea can reclaim restful slumber and embark on a path toward enhanced health and well-being.
Unlock the secrets to deep, restorative sleep with our expert guidance and support. Don’t wait any longer—book your appointment now to begin your transformational journey towards better sleep and better health.