Sleep apnea is one of the most common health conditions that keep people from having a sound sleep at night. Statistically, one in every 15 Americans suffers from sleep apnea. Sadly, most of these people aren’t even aware of this issue.
Fortunately, sleep apnea is curable, but there are different types of sleep apnea. Today, we’ll focus on understanding central sleep apnea treatment options because it’s one of the most common forms of the issue.
But first, we’ll share more details on what central sleep apnea is, central sleep apnea symptoms, causes, and more for your better understanding. So, let’s get right to it!
What is Central Sleep Apnea?
Central sleep apnea CSA is a health condition that leads to periodic breathing patterns where the patient experiences a lack of ventilation. While this doesn’t necessarily wake the patient up, it does keep him from experiencing sound sleep. Thus, he or she might suffer from a myriad of problems in daily life.
Central Sleep Apnea Causes and Types
Central sleep apnea syndrome is when a person stops breathing during sleep. But, why does it happen in the first place? Well, there’s a condition where your brain’s ability to maintain ventilatory effort reduces. So, at times, your brain doesn’t send signals to your muscle relaxants, thus stopping the breathing patterns.
However, there are other types of sleep apnea as well. Apart from central sleep apnea, we have obstructive sleep apnea and complex sleep apnea. Central sleep apnea and obstructive sleep apnea are very different from one another, while complex apnea is a combination of the two.
Then again, there are different types of central sleep apnea CSA as well. The types of central sleep apneas are as follows:
Cheyne-Stokes Breathing
A person suffering from Cheyne stokes breathing pattern will start speeding their breathing speed up, but will slow down and eventually stop until they start breathing again. This cycle usually repeats and can last up to 2 minutes.
Most people suffering from central sleep apnea suffer from Cheyne stokes breathing. However, it’s most common in stroke and heart failure patients.
Narcotic-Induced Central Sleep Apnea
There are different narcotic-based medications that can lead to central sleep apnea. For example, most Opioid-based medications such as morphine, codeine, and oxycodone can affect your breathing pattern during sleep, so it’s better to avoid them.
High Altitude Periodic Breathing
High altitude periodic breathing is experienced by a lot of people when they ascend a certain height over sea level. Usually, it’s experienced when someone climbs above 8,000 feet or 2,500 meters.
Treatment-Emergent Central Sleep Apnea
Treatment-emergent apnea is caused due to certain medical procedures. What’s ironic is, some people undergoing positive airway pressure treatment for curing obstructive sleep apnea will experience central sleep apnea. While the percentage is as low as 10%, it’s still a possibility.
Medical Condition-Induced Apnea
Certain medical conditions such as kidney failure, stroke, heart failure, Parkinson’s disease, etc. can cause central sleep apnea.
Idiopathic Central Sleep Apnea
Also known as Primary central sleep apnea, Idiopathic central sleep apnea is still being researched and there isn’t any conclusion as to why this happens. However, it’s closely related to congenital central hypoventilation syndrome, also known as Ondine’s curse.
What’s the Difference? – Obstructive Sleep Apnea vs. Central Sleep Apnea
Obstructive sleep apnea is also commonly seen among patients. However, unlike central sleep apnea, obstructive sleep apnea leads to abnormal breathing patterns due to something obstructing the respiratory tract.
OSA can be caused by various issues. The most common reason is a patch of overgrown tissue blocking the nasal cavity when the muscles are relaxed. It can also be caused due overgrown flesh in the nasal cavity, or even a large tongue.
One of the major differences between OSA and CSA is, sufferers of OSA get a signal from their brain that helps them wake up when their breathing patterns stop. However, sufferers of CSA don’t get this signal. So, even if they start choking in their sleep, their chances of waking up are low.
They can only hope that their brain will start sending signals again to stimulate breathing, or their bed partner will wake them up. This is why doctors can treat obstructive sleep apnea more easily and it has a lower fatality rate.
Central Sleep Apnea Symptoms
Central sleep apnea CSA can lead to various sleep disorders. These are:
- Abnormal breathing patterns during sleep or periods of not breathing in case of severe central sleep apnea
- Fatigue, which can lead to difficulty concentrating during the day
- Excessive daytime sleepiness, or hypersomnia, is also commonly found in central sleep apnea patients
- CSA patients often suffer from mood changes due to the fatigue
- Snoring is a common problem that’s seen in almost every sleep apnea patient, but that doesn’t necessarily mean that you have sleep apnea if you snore
- Central sleep apnea patients often suffer from morning headaches
- High blood pressure
Who Is at Risk for Central Sleep Apnea?
Anyone can be affected by central sleep apnea. It’s more common among the elderly and also among people with certain medical conditions. Also, it’s found that men are more likely to be inflicted by central sleep apnea than women.
Here are some conditions that have been linked to central sleep apnea over the years.
- Kidney failure
- Congestive heart failure
- Hypothyroid disease
- Neurological diseases
- Damage to the brainstem from swelling
How Is Central Sleep Apnea Diagnosed?
The first person to notice central sleep apnea is not the sufferer himself, but his bed partner. So, if you’re living alone, it might take more time for you to realize that you’re suffering from central sleep apnea.
If you’re facing the sleep disorders we discussed earlier, then it’s time for you to visit a sleep clinic that can diagnose your condition. Usually, the sleep expert inquires about medical history, and sleep history, and conducts a thorough physical exam.
There are different kinds of examinations, but usually, the following are tested:
- Brain’s electrical activity
- Eye movement during REM sleep
- Muscle activity of your respiratory tract during sleep
- Heart rate
- Breathing during sleep
- Air pressure in your respiratory tract
- Blood oxygen level
Depending on the number of times you’ve stopped during sleep, the expert will determine the severity of your sleep apnea. With clinics like SleepApneaTreatment, you can get these done at your home even!
Treatments for Central Sleep Apnea
There are different ways of treating central sleep apnea. In fact, there are so many alternatives that patients often find themselves confused. In this section, we’ll go through all of them and drop our suggestions regarding which path you should take.
Taking care of Associated Medical Conditions
As discussed, certain health conditions can lead to central sleep apnea. If these conditions are treated, then it might ease sleep apnea to some extent. For example, a patient suffering from heart failure can decrease the risks of suffering from central sleep apnea by getting therapy for the underlying cause.
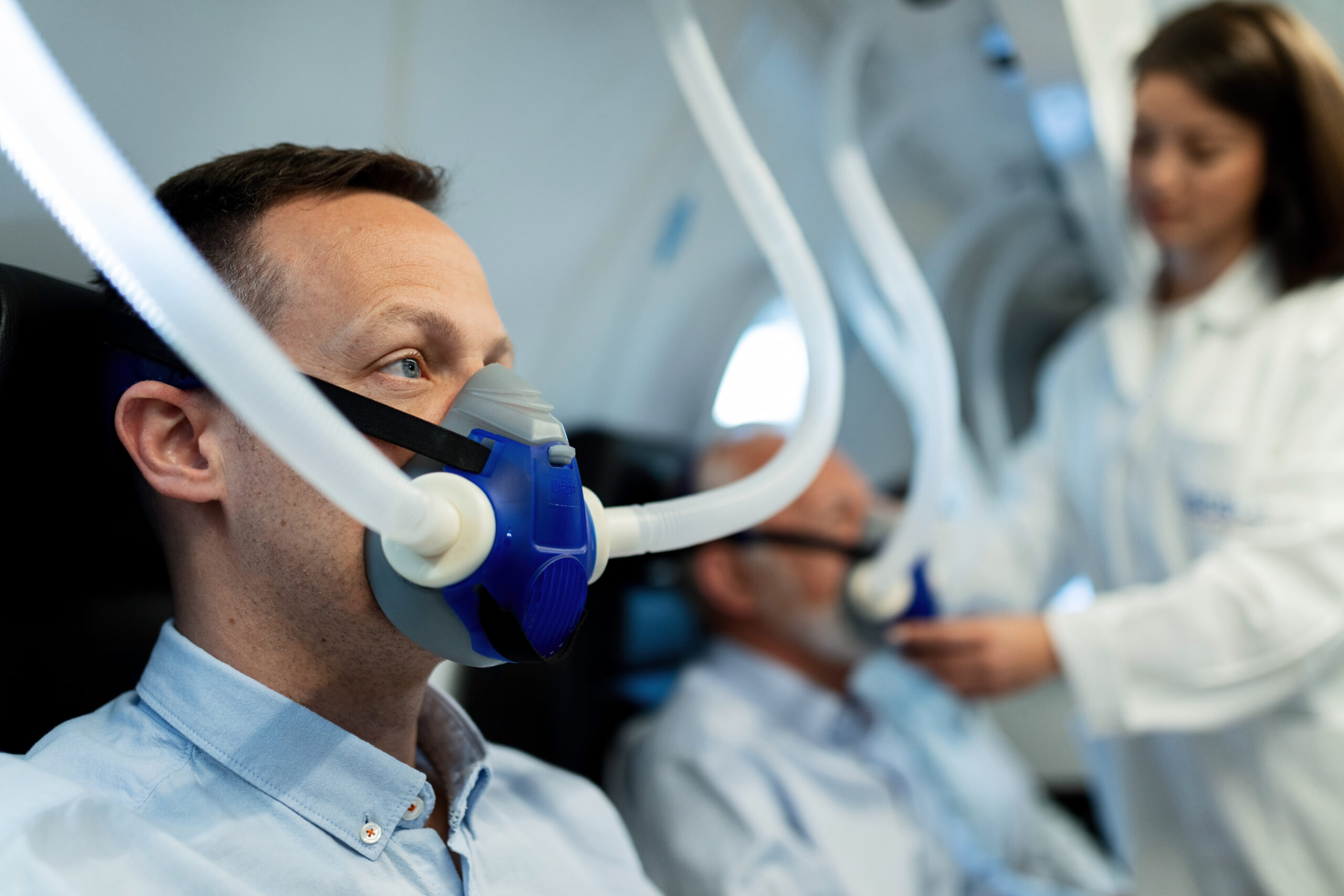
Continuous Positive Airway Pressure (CPAP)
Continuous positive airway pressure treatment is a popular treatment for sleep apnea. In this therapy, you’re required to wear a mask that covers your nose, mouth, or both.
In continuous positive airway pressure therapy, constant air pressure is maintained in your respiratory tract by supplying air through the mask. This is capable of preventing your respiratory instability, thus allowing you to maintain regular breathing during sleep.
Adaptive Servo-Ventilation
While CPAP is a treatment procedure capable of helping you with central sleep apnea, it might not work for everyone. In that case, the doctors will subject the patients referred to ASV or Adaptive servo-ventilation.
ASV is actually an advanced version of CPAP. While CPAP maintains a steady air pressure throughout time, ASV changes the air pressure on cyclic patterns.
So, it can essentially stimulate breathing. Even if you don’t move a muscle, you’ll still be breathing with an ASV on. That being said, ASV only helps in inhaling and doesn’t play any role when you’re exhaling.
Also, ASV isn’t appropriate for people suffering from systematic heart failure.
Bilevel Positive Airway Pressure (BPAP)
BPAP is an even more advanced procedure than ASV. While ASV is capable of changing the positive airway pressure when you’re breathing, Bilevel positive airway pressure, or BPAP can also help you exhale.
This means, it will not only help you inhale, but it’ll also help you in exhalation. In fact, some of the advanced BPAP machines can be programmed to deliver you a breath if you haven’t breathed for a certain time.
Then again, BPAP isn’t great for people suffering from heart failure. So, it should only be used with discretion.
Supplemental Oxygen
Supplemental oxygen can also help with central sleep apnea. However, you’ll be missing out on features such as variable positive airway pressure offered by CPAP, ASV, or BPAP. This is why this treatment procedure isn’t that favored by physicians.
Medications
There are certain medications such as acetazolamide that can help stimulate breathing while you sleep. These are mostly offered to people who can’t tolerate positive airway pressure that devices like CPAP and BPAP function on.
Surgery
There’s this new therapy procedure for curing central sleep apnea, and it’s called transvenous phrenic nerve stimulation. This system has recently been approved by U.S. Food and Drug Administration, but it’s still in its early stages.
In this procedure, a chip is implanted just underneath the upper chest of the patient. This chip sends an electrical pulse to the brain to maintain a steady respiratory effort. When the signal is sent to the brain, the brain sends a signal to the diaphragm, thus instructing it to take a breath.
While this works great for people suffering from moderate sleep apnea, it’s still uncertain how this can help people with severe central sleep apnea.
Oral Appliances
While the mentioned procedures can be effective for many, they’re too expensive or not good enough. For example, while BPAP, CPAP, and ASV are amazing, they’re very expensive, aren’t suitable for people who can’t withstand positive airway pressure, and pose an increased risk of heart failure.
On the other hand, cheaper options like supplemental oxygen may not work, and medications can have side effects if used for a long time.
This brings us to oral appliances. These devices can help a person maintain steady breathing, are cheap, and are quite effective.
Vivos Sleep Apnea Treatment
Speaking of oral appliances, we had to mention the Vivos sleep apnea treatment. This is offered by SleepApneaTreatment clinic, the same clinic that facilitates sleep apnea diagnosis at your home.
The best part about Vivos sleep apnea treatment is that it’s completely non-invasive. You don’t have to spend a ton, and it has great chances of success.
So, how does it work? For this to work, you will have to wear an appliance from Vivos. The appliance is designed to apply a light pressure on your palate so your breathing remains consistent throughout the night.
One of the best things about the Vivos treatment is that it addresses the root cause of sleep apnea for many, which is jaw positioning.
The appliance will slowly change your jaw position. It takes the appliance about 18 months to heal sleep apnea completely.
Conclusion
Central sleep apnea isn’t fatal only, but it can also hamper your productivity and lifestyle with daytime drowsiness, disrupted sleep, unstable ventilatory control, and more.
If you could relate to some of the symptoms we’ve discussed today, you should get central sleep apnea diagnosed by a professional.
To do so, simply contact SleepApneaTreatment as you won’t even have to leave your home to get diagnosed. Rather, they’ll send a professional who’ll conduct the diagnosis at your home.
Among all the treatments discussed, the Vivos treatment is the most effective, safest, and affordable. So, we highly recommend trying that out.