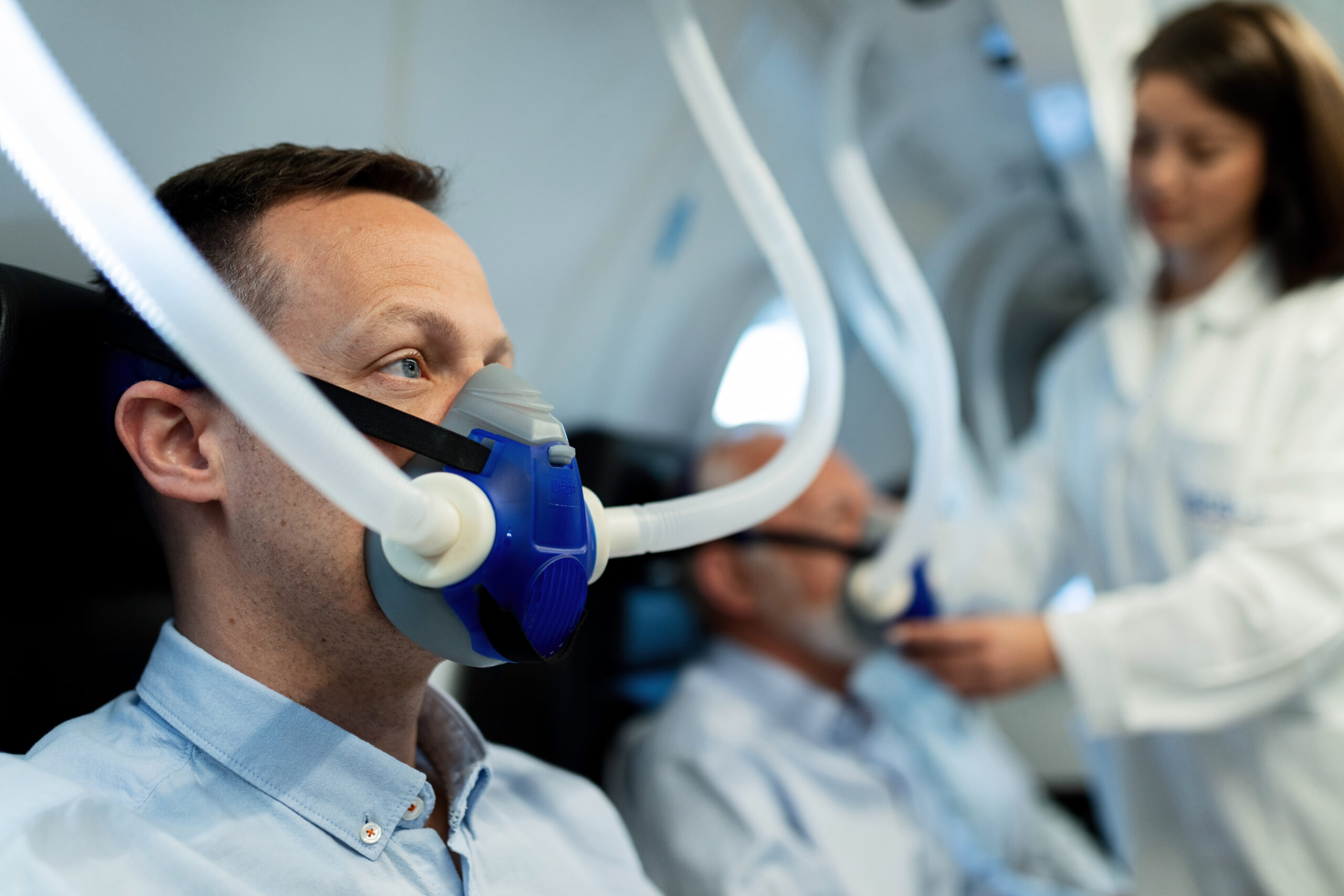
Central sleep apnea (CSA) is a disorder that systematically stops your breathing during sleep.
Unlike obstructive sleep apnea (OSA) when the issue is a blocked airway, CSA occurs because the brain does not communicate with the muscles properly. Since the breathing muscles don’t receive brain orders, they don’t take in air as they should. This chain reaction leads to repeated breathing pauses.
CSA may not seem like a big deal, and some could consider it a mild inconvenience. However, this disorder is the consequence of underlying health conditions. Drowsiness, inability to rationalize and fragmented sleep are only a few problems that come with CSA.
What Are Common Central Sleep Apnea Symptoms?
Repeated interruptions in your breathing while sleeping is a giveaway of CSA. The following are other symptoms that trace back to this disorder.
· Elevated tiredness during daytime.
· Frequent awakenings while sleeping at night.
· Regular headaches experienced during the morning.
· Issues to concentrate properly.
· A lower desire for sexual engagement.
· Memory problems and mood swings.
· Lack of sleep and potential insomnia.
· Inability to work out.
One thing to consider is that CSA does not usually produce snoring problems. This symptom is more likely to happen when you experience obstructive sleep apnea.
Central Sleep Apnea Types & Causes
Central sleep apnea and its cause vary depending on the type. This disorder can happen naturally (primary central sleep apnea), or as the result of another condition (secondary central sleep apnea).
Primary CSA is the rarest type, and there’s no clear cause for it in adult patients. Secondary central sleep apnea types are easier to identify because breathing interruptions are the result of an existing health condition.
These are the most common types of CSA sleep disorders with their usual characteristics and causes.
· Cheyne-Stokes Breathing
This CSA type is the most common, usually tied to congestive heart failure, strokes, and other heart conditions. Typically, Cheyne Stokes breathing involves a sudden increase and decrease of airflow speed followed by a long pause.
· CSA Induced By a Medical Disorder, But No Cheyne-Stokes Breathing
You may develop CSA without the common symptoms of Cheyne-Stokes breathing. In this case, the reason is a preexisting health condition, usually brain stem injuries.
· CSA Induced By Medication or Substance Use
The use of medication like opioids can affect your breathing consistency. Airflow may increase, decrease, or stop entirely. Methadone is the drug most related to this condition.
· High Altitude Periodic Breathing
In this condition, you may react with a Cheyne Stokes breathing pattern at high altitudes. Oxygen levels change at considerable heights, producing inconsistent breathing between hyperventilation (quick breathing), and slow breathing.
· Treatment Emergent Central Sleep Apnea
When you undergo treatment for obstructive sleep apnea such as positive airway pressure, you might develop this type of CSA. Only 5% to 15% of patients undergoing positive airway pressure treatment suffer from this condition.
Central Sleep Apnea Risk Factors
Anyone could suffer sleep related breathing disorders like CSA. However, scientific research proved that some individuals are more likely to develop this condition. These factors often contribute to central sleep apnea syndrome.
· Age
CSA is more prone to develop in individuals over the age of 65. The reason could be natural aging and the likelihood of older people suffering heart conditions and illnesses related to the brain and blood vessels.
· Gender
Males are more likely to experience central sleep apnea syndromes. The reason could be testosterone’s impact on the carbon dioxide built up within the blood until the next breath taken.
· Medical Conditions
Atrial fibrillation produces irregular heartbeats, and congestive heart failure leads to a lack of enough blood pumping. These two conditions produce CSA. Brain conditions can also affect your ability to breathe properly, whether it’s a stroke, brain tumor, or brainstem injury.
· Use of Medication
Opioids, antidepressants, and muscle relaxants increase central sleep apnea risks. Other medicine like anticonvulsants and benzodiazepines can also produce CSA.
· Continuous Positive Airway Pressure for Obstructive Sleep Apnea Treatment
If you experience obstructive sleep apnea and undergo continuous positive airway pressure treatment, you could develop central sleep apnea. This variation is a combination of both disorders, usually called complex sleep apnea.
Central Sleep Apnea Diagnostic
If you believe you have central sleep apnea, a healthcare provider can diagnose the disorder by evaluating different factors. Doctors will require your medical history and a detailed description of the symptoms. They will ask for a physical exam and suggest a sleep history.
Some factors doctors evaluate are whether you deal with breath interruptions, incapacity to breathe while lying on your back or sides, and abrupt awakenings at night. CSA does not have a specific physical symptom, but all these signs point to the disorder.
Polysomnography, a Sleep Study to Confirm Central Sleep Apnea
Once the doctor has high suspicions you may be dealing with CSA, they will refer you to a sleep laboratory. In this facility, professionals carry out sleep studies overnight to confirm whether the individual has CSA. The name of this study is polysomnography.
Polysomnography is a study that evaluates physical functions while sleeping. Scientists use sensors attached to different body parts, like the head and chest. These sensors measure multiple activities, such as:
· Multiple sleeping phases.
· The effort needed to breathe.
· How much air goes in and out.
· Oxygen level within the bloodstream.
· Heart functions, rate, and rhythm.
The person in charge of the study evaluates whether you stopped breathing, how long it lasted, and the number of interruptions. This data allows them to rate the severity of your sleep breathing disorder.
Central Sleep Apnea Treatment
Since most CSA types are the result of a different health condition, the treatment purpose is to target the root cause. Doctors could also recommend medication or other treatments to stimulate breathing and regulate it while sleeping.
The approach also varies depending on the CSA severity. If you experience mild complications, taking care of the underlying cause could be enough to restore continuous breathing patterns.
When the condition is more severe and includes blood flow or heart issues, the treatment is different. In this case, doctors may recommend treatment to take care of the medical condition and the CSA itself.
Treatments recommended for central sleep apnea include:
· Continuous Positive Airway Pressure (CPAP)
Under this treatment, a machine introduces a constant airflow stream through a mask into the nose and mouth while sleeping. Variations of this treatment include adaptive servo ventilation, also called ASV, and bilevel positive airway pressure, denominated as BPAP.
· Complementary Oxygen Treatment
This treatment includes using a machine to pump oxygen into the lungs. Normally, this procedure is for people that did not improve with PAP therapy.
· Use of Medication
Generally, medication is the third option when other treatments fail. The purpose of the medicine is to stimulate breathing, and they may include side effects. Therefore, professional supervision is necessary.
· Stimulating the Phrenic Nerve with a Device
When common treatments do not work, doctors could recommend using a device implanted in the chest surgically. The purpose of this device is to emit signals into the nerve responsible for stimulating your diaphragm. As a result, the diaphragm will contract as it should for regular breathing.
Complications of Central Sleep Apnea
If you believe you suffer from CSA, act quickly and consult a doctor. This disorder can lead to other complications that will affect your daily activities. For example:
· Excessive Fatigue
Sudden and repeated awakenings during your sleep will not allow you to rest, causing excessive fatigue. You will also experience irritability, and could potentially fall asleep at work or while driving. These issues can put you and others in danger.
· Cardiovascular Issues
One effect of experiencing central sleep apnea is that the body losses blood oxygen levels constantly. Without proper treatment, this condition can affect your heart health significantly. For instance, this syndrome could produce abnormal heart rhythms.
What to do Following Central Sleep Apnea Diagnosis?
A central sleep apnea diagnostic can be a relief. After all, you finally discovered what’s keeping you from enjoying a good night’s rest. Fortunately, living with this condition is possible and the treatments work to provide an effective cure. Here’s what you can do to make things easier.
· Educate Yourself on CSA
Central sleep apnea and sleep disorders in general can have multiple causes, making them harder to understand. Therefore, take the time to learn about the disorder, its symptoms, and which treatment you should follow. Multiple websites and forums discuss this disorder and can be helpful.
· Avoid Preventable Causes
Some factors like high altitudes, use of opioids, and alcohol consumption can cause CSA. Thus, avoiding these triggers is a simple and effective method to prevent central sleep apnea. If your medication is the cause of your sleep disorder, talk to your doctor about potential alternatives.
Final Words
Central sleep apnea can be a severe sleep disorder, but multiple treatments exist to take care of it. If you suspect you have this condition, talk to a doctor or specialist on how to proceed. With proper care and special attention, living with CSA is possible and the condition is curable.