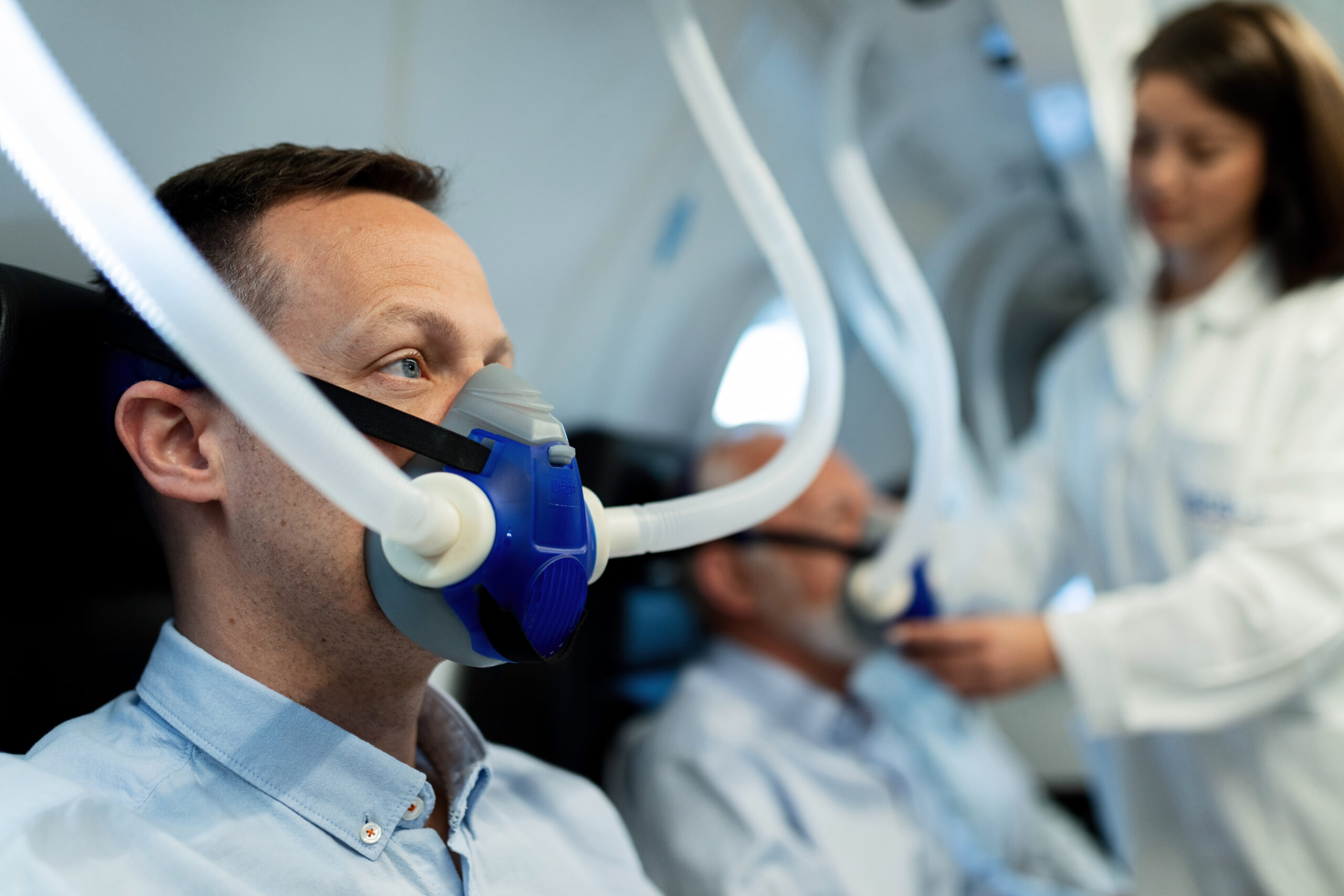
Obstructive sleep apnea, commonly abbreviated as OSA, is a sleep disorder. When you have this condition, you experience upper airway blockage and force your body to work harder to breathe air.
OSA produces shallow breathing and could interrupt airflow into your lungs. Following a short interruption, you resume your breathing with an audible gasp or snort.
While these symptoms are not noticeable when you sleep, obstructive sleep apnea affects your ability to rest properly. In other cases, OSA affects oxygen flow and has a negative impact on your heart rhythm.
What Exactly is Obstructive Sleep Apnea?
Obstructive sleep apnea is a disorder resulting from repeated upper airway collapse while sleeping.
Normally, obstructive sleep apnea occurs following complete relaxation of the muscles that support throat soft tissues. Under this reaction, your airway narrows or shuts down and interrupts your capacity to breathe.
Therefore, air does not flow within your respiratory tracks and into your lungs as it should.
Obstructive sleep apnea often causes snoring, resulting from the airflow entering the tight airway space. However, snoring is not always a symptom of this disorder.
Obstructive Sleep Apnea Symptoms
When you suffer obstructive sleep apnea while sleeping, the brain notices your sleep disordered breathing and forces you to wake up. Awakening in this manner allows your body to restore your airway.
Sometimes, this action is subtle enough that you don’t remember it. However, the same activity can occur all night long, keeping you from resting. During the daytime, you will feel sleepy without knowing that you didn’t sleep well.
Therefore, you must know how to identify other signs and symptoms that could hint at OSA. For instance, you may be dealing with this disorder if:
· You deal with excessive daytime sleepiness.
· A family member or bed partner notices loud snoring.
· Another person sees that you stop breathing while sleeping.
· You experience sudden awakenings, followed by gasping or choking.
· Your mouth is dry, or your throat is sore after waking up.
· You feel headaches in the morning and have issues concentrating during daily activities.
· You go through sudden mood changes, feeling sad or infuriated for no apparent reason.
· Your blood pressure is high.
· Your sex drive is low.
Children can also develop obstructive sleep apnea. In this case, some noticeable symptoms are the following:
· The child wets the bed.
· Drooling or choking issues.
· Excessive sweating at night.
· Contraction of the ribcage while exhaling.
· Uncommon behavior and learning problems.
· Sleepiness.
· Snoring, grinding of teeth, and interrupted breathing.
Remember that these are all potential signs of obstructive sleep apnea syndrome. Learn more about the risk factors for more evidence.
Obstructive Sleep Apnea Risk Factors
While almost anyone can develop sleep disorders like OSA, some factors increase your likelihood of having this condition.
· Overweight. Not all people with overweight suffer from OSA, but excess weight can result in fat deposits accumulation near the upper airway area. Thus, the risks of breathing obstruction are higher. Conditions related to obesity, like hypothyroidism, also are likely to cause OSA.
· Age. The risk of developing OSA increases with age.
· A Naturally Compressed Airway. It could be the case that you inherited narrow airways naturally. Alternatively, your tonsils and adenoids could increase in size, blocking your airway. Family OSA history also increases risks.
· Hypertension. If you have high blood pressure, you face more risks of developing OSA.
· Gender. Both genders can develop OSA under specific circumstances. Men are normally more prone to this condition, but women also can develop the disorder after menopause.
· Asthma and Diabetes. Research shows that OSA can be more common if you have diabetes or asthma.
Obstructive Sleep Apnea Diagnosis
When you suspect you suffer from OSA, your doctor can determine whether or not the disorder is present. First, the doctor will require an examination of your medical history and physical condition. Elements like daytime sleepiness and snoring records are usually very helpful.
Afterward, the doctor will perform exams to check your head and neck area. This exam allows the doctor to spot any physical signs often linked to sleep apnea.
Once your doctor considers them necessary, they will require tests to confirm the obstructive sleep apnea diagnostic.
Polysomnography
Polysomnography or PSG is a test that studies your bodily functions while sleeping. This study requires you to sleep at a hospital or laboratory with multiple sensors attached to your head, chest, and other body parts. The purpose of these sensors is to track physiologic behaviors.
A PSG test tracks the activity of many organs related to your sleeping cycle, including:
· Brain waves.
· Eye movement.
· Muscle activity.
· Heart rate and rhythm.
· Blood oxygen levels.
Obstructive Sleep Apnea Treatments
Different treatments exist to prevent airflow blockage by OSA while sleeping. Depending on your condition, the doctor could recommend the following options.
· Continuous Positive Airway Pressure (CPAP)
This treatment is usually the first option when it comes to treating OSA. While undergoing CPAP, a machine administers oxygen through a mask into the mouth and nose during sleep. By delivering positive airflow pressure, the machine and the mask maintain open airways.
Sometimes, this treatment may not provide the desired results. Oral appliances could be an alternative if CPAP therapy fails.
· Bilevel Positive Airway Pressure (BPAP)
If CPAP does not work, the next treatment option is BPAP. This therapy also consists of machines that deliver oxygen in two pressure settings depending on your breathing habit. Therefore, the technician can adjust the pressure for inhaling and exhaling.
· Positional Therapy
This type of therapy refers to sleeping on your side instead of over your back. Sometimes, OSA produces more discomfort when lying down while facing up. Positional therapy teaches you to sleep on your side if you have mild sleep apnea when sleeping on your back.
· Surgery
Severe obstructive sleep apnea caused by natural or accidental upper airway blockage may require surgery. Normally, this method to cure OSA is the last treatment option when CPAP and BPAP don’t work. However, some conditions apply. For instance:
Ø You’re willing to undergo surgery.
Ø The problem blocking your airway is correctable via surgery.
Ø Your physical condition is optimal to withstand surgery.
If you meet the requirements, your doctor will request a physical exam to evaluate the condition of your upper airway. Depending on the problem, the doctor may recommend somnoplasty, and nasal or mandibular advancement surgeries, to name a few.
· Other Methods to Treat Obstructive Sleep Apnea
Surgery may not be necessary if the OSA is mild to moderate. Sometimes, you can treat this and other sleep disorders like central sleep apnea by implementing a few measures.
Losing weight. Even a small amount like 10% of weight loss can improve your sleep disorder.
Avoid drinking alcohol and taking sleep medicine. These substances are more likely to shut your airway while sleeping, incapacitating your ability to breathe normally.
Using nasal sprays. If you have trouble breathing at night due to sinus or nasal congestion, a nasal spray can help.
Getting an oral device. Some devices for mandibular advancement control your tongue to avoid throat blocks. As a result, your airway remains open during sleep.
Obstructive Sleep Apnea Complications
Not treating OSA accordingly can affect you and those around you in many ways. For example:
· Higher risks of accidents. OSA causes a lack of concentration, which is dangerous while driving vehicles or working in dangerous fields. Children also are more prone to accidents due to a lack of surrounding awareness.
· Cardiovascular problems. Unusual sleeping patterns can affect more than your resting hours. Since this disorder causes drops in blood pressure, you could suffer from heart attacks, elevated blood pressure, and irregular heart rhythms.
· Problems with family or bed partners. OSA produces loud snoring, which can keep those close to you awake during the night. Sleep-deprived partners will not rest well and may experience sleepiness and lack of concentration during the day.
· Other complications caused by this disorder include glaucoma, dry eye, metabolic disorders, and pregnancy problems.
Is Obstructive Sleep Apnea the Same as Central Sleep Apnea?
Obstructive sleep apnea (OSA) and central sleep apnea (CSA) are not the same disorder.
The cause of obstructive sleep apnea is airway blockage, produced when muscles at the end of the throat relax and prevent normal breathing. In this situation, your airway can narrow or shut down and lead to airflow interruptions for 10 seconds or longer.
On the other hand, central sleep apnea occurs when your brain cannot communicate with your breathing muscles properly. This lack of brain signal reception prevents muscle functions to pull air into your lungs. As a result, you experience repeated breathing interruptions.
Some symptoms and treatments are similar for both disorders.
However, consulting with your doctor is necessary to identify the correct approach. In some cases, people develop treatment emergent central sleep apnea after undergoing positive airway pressure treatment for OSA. The resulting disorder is what specialists call complex or severe sleep apnea.
Final Words
Untreated obstructive sleep apnea is serious and can affect your lifestyle in numerous ways. From precarious health conditions to accident risks and strained relationships, this disorder is no joke. Some people don’t even notice they have OSA, as some symptoms often pass as normal.
Therefore, a comprehensive diagnostic is the right approach if you experience one or many symptoms.
Consult with your doctor to have your obstructive sleep apnea diagnosed. A specialist will determine what actions to take and which treatment is the most appropriate for your condition. Living with obstructive sleep apnea can be frustrating, but it doesn’t have to be temporary.